Folliculitis Causes, Symptoms & Treatments
Folliculitis is the inflammation of the hair follicle. It is a common skin condition where pinpoint red bumps appear on the surface of the skin. It can be either infectious (i.e. bacterial) or noninfectious (i.e. trauma or occlusion of the follicle). Each bump involves a hair follicle, and within its walls, inflammatory cells can accumulate creating a pustule in the base of the follicle. It can affect any individual regardless of age, race, or gender. The common areas involved are usually the face, chest, back, scalp, buttocks, groin, thighs, and legs. It will not involve areas where there are no hair follicles. It is often seen even in healthy individuals and is easily treatable. In some cases, it may even resolve on its own.
The treatment of folliculitis depends on the cause and severity of the condition. Patients with diabetes, altered immune status (i.e. cancer or AIDS patients), malnutrition, obesity or using certain types of medications (i.e. topical steroids) are at higher risk for developing folliculitis.
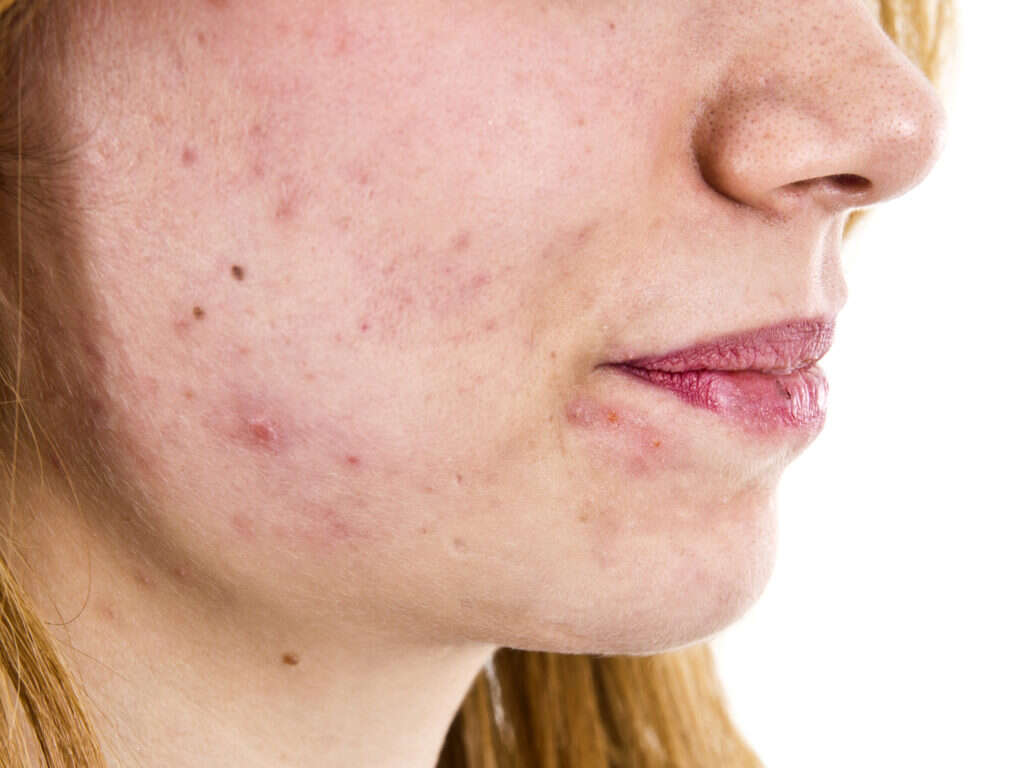
Cause #1: Bacterial Infection
Folliculitis can be caused by a bacterium known as Staphylococcus aureus. It is a bacterium than can be often found on the skin. This type of folliculitis is superficial and often has itchy, white, and pus-filled bumps. Although Staphylococcus aureus is the most common etiology, other bacteria can cause folliculitis as well. Certain gram-negative organisms (i.e. Enterobacter, Klebsiella, Escherichia) can cause folliculitis on patients that have been treated for acne with long-term systemic antibiotics. Another gram-negative folliculitis (also known as hot tub folliculitis) can be caused by a type of bacteria known as Pseudomonas. This form of folliculitis may be associated with systemic symptoms (i.e. fever).
Depending on the severity of the infection, an antibacterial wash, a topical antibiotic, or oral antibiotic can be prescribed. For uncomplicated superficial lesions, the administration of antibiotics may not be necessary. However, for refractory or deep infectious lesions systemic antibiotics might be indicated. In some cases, Staphylococcus aureus resistance to certain antibiotics (i.e. penicillin or even methicillin-resistant) can be present, thus leading to the empiric use of antibiotics of a wider spectrum.

Cause #2: Fungal infection
While fungal folliculitis is not as common as bacterial folliculitis, it can also occur. Folliculitis that is caused by a fungal infection is most commonly due to the yeast Malassezia furfur. It is known as a Pityrosporum folliculitis and it usually presents as an itchy eruption of red and pus-filled lesions in the upper trunk of young adults. Lesions can also be present in the shoulders, neck, arms, and face.
Moreover, superficial folliculitis can also be caused by a dermatophyte infection known as tinea barbae, especially in the areas of the face and neck of adult males.
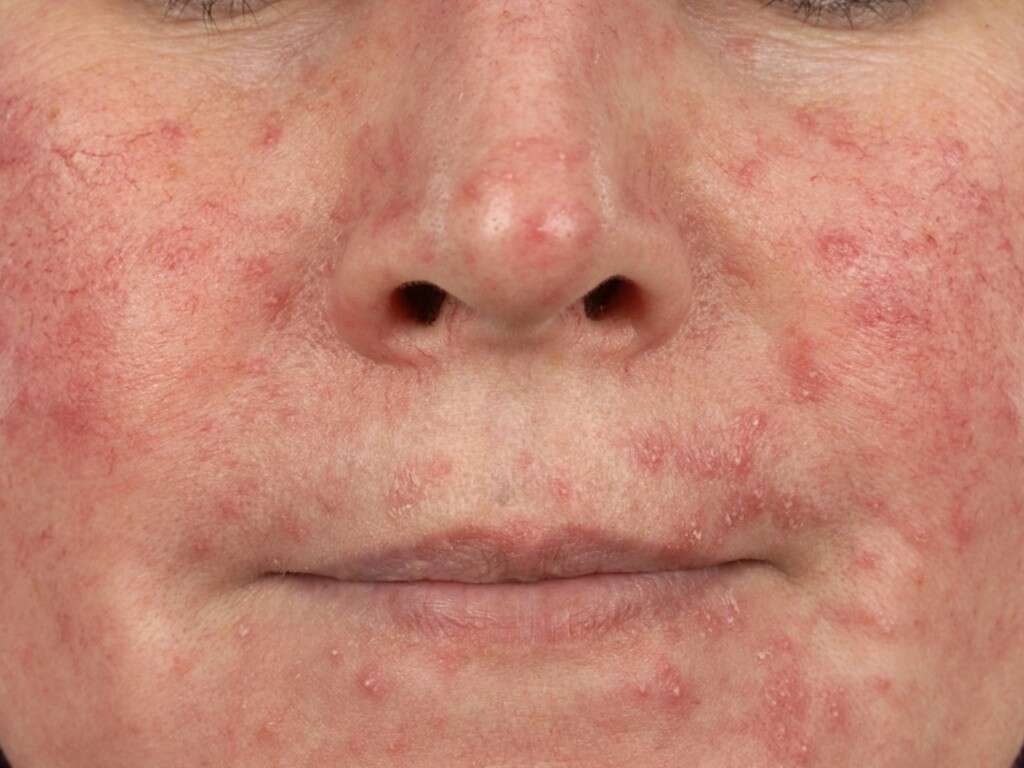
Cause #3: Viral Folliculitis
Folliculitis is frequently caused by bacteria. However, viral folliculitis can also be observed, though relatively uncommon. It can be caused by herpes simplex viruses or varicella-zoster virus. Folliculitis caused by herpes simplex viruses (1 and 2) usually spreads by shaving and appears as multiple vesicles on the affected skin.
Varicella-zoster virus can affect follicles causing lesions that appear according to dermatomes or the area of the skin supplied by a single spinal nerve (dermatomal distribution).

Symptom #1: Bumps
In folliculitis, there are clusters of red bumps that are individual hair follicles seen on the affected area. These bumps are filled with pus and can vary in size, ranging from 2 to 5mm. Some patients may even confuse them with yellow or white-headed pimples. In a staphylococcus infection, it can become crusty.
Depending on the cause of folliculitis, it will determine which areas are most commonly affected. Spread may occur to the surrounding areas.
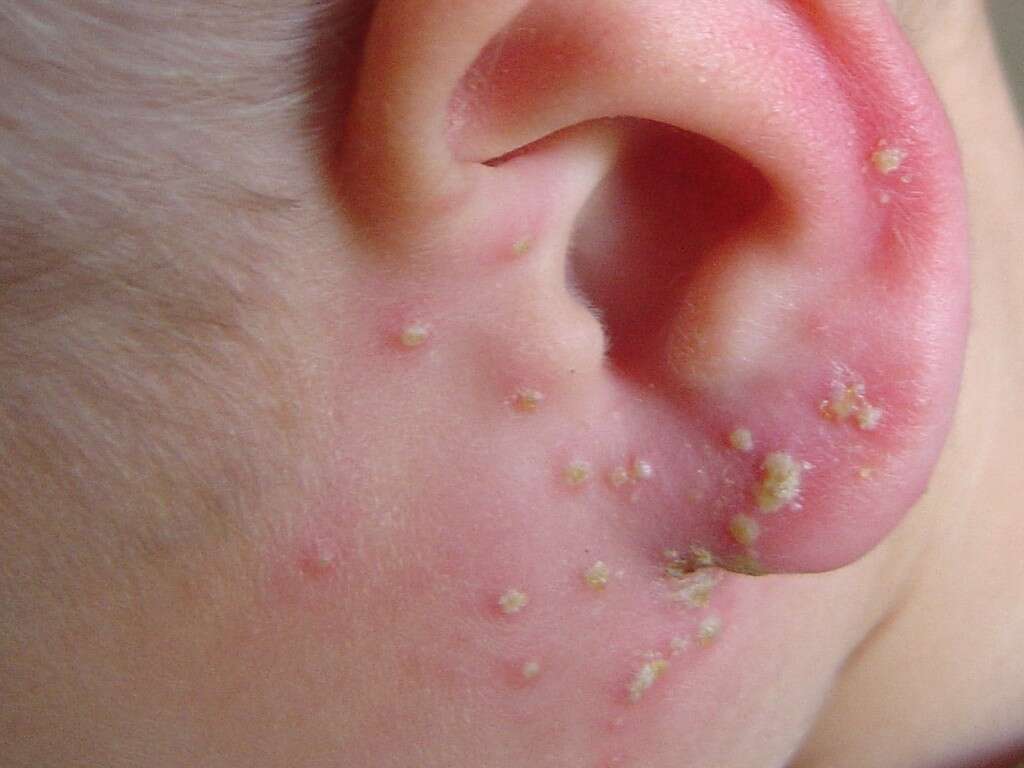
Symptom #2: Itchiness
In most forms of folliculitis, the area of the infected skin can become red, inflamed, and itchy.
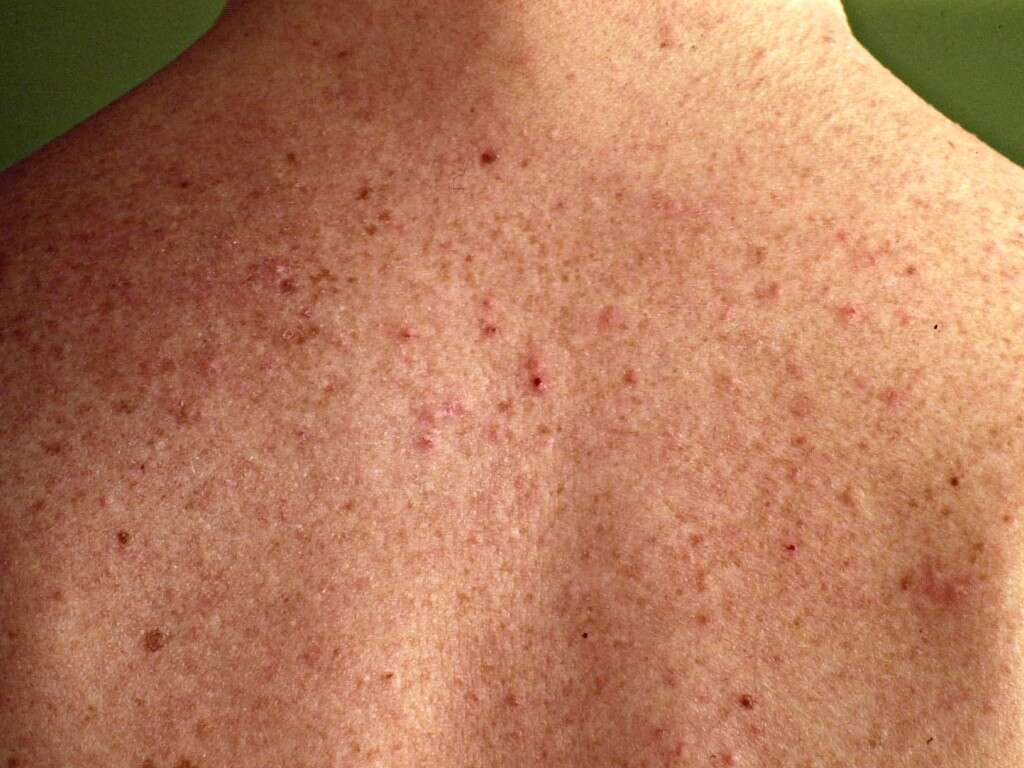
Folliculitis, caused by the fungi Pityrosporum (Malassezia furfur), usually presents with intensive itchiness in the back, shoulders and chest.
Symptom #3: Discomfort
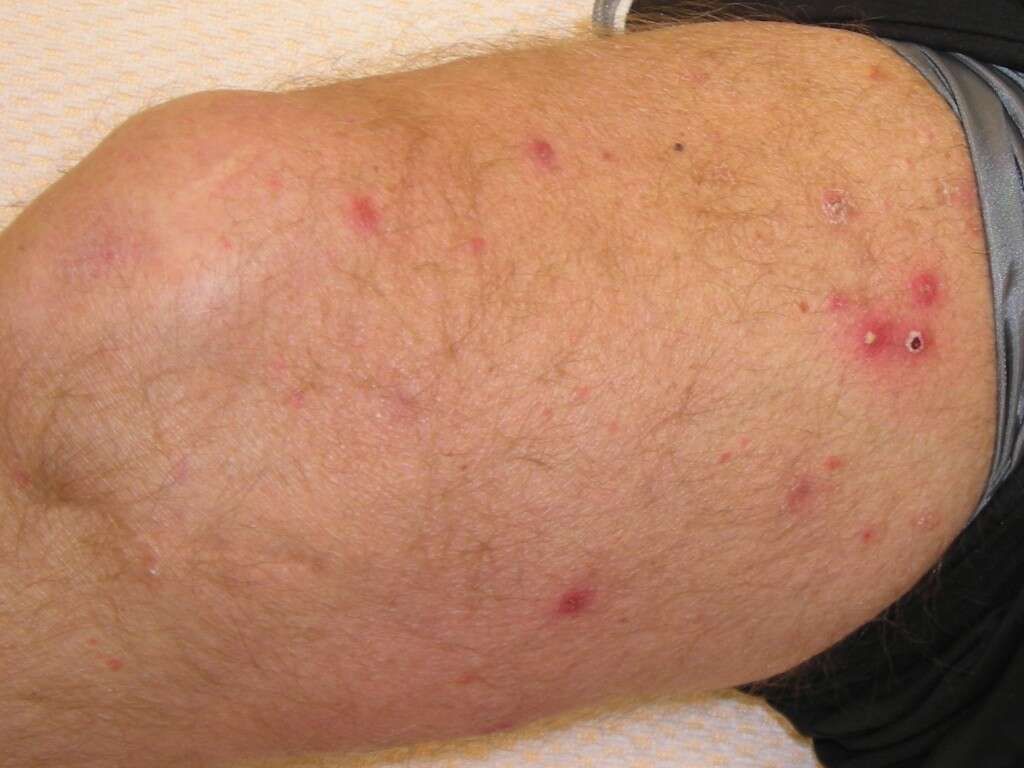
Folliculitis can cause the affected area to become painful, and swollen. You may also feel a burning sensation and tenderness. All these are caused by the inflammation of the hair follicles that are filled with pus. Mild and moderate cases often feel tender and itchy while in severe folliculitis, the infection can be deeper and possibly involve the entire follicle.
Severe infections are often painful and can lead to complications such as the infection of the deeper layers of the skin (i.e. cellulitis), scarring, and even permanent hair loss. If you suspect that you have a more severe form of folliculitis, you should seek medical attention as soon as possible to avoid complications.
Treatment #1: Antibacterial Wash
In mild cases of folliculitis, your physician may recommend over the counter antibacterial wash (i.e. twice daily). Most cases that are mild will eventually self-resolve. The antibacterial wash helps prevent further infection and cleanses the infected area.
Avoid using an antibacterial wash that is too harsh on the skin. Wash the area gently and try not to scrub it roughly as it can irritate the area which leads to more redness and inflammation. If your face is affected, your doctor will probably recommend an antibacterial wash that is labeled specifically for facial use as it is gentler compared with others.

Treatment #2: Soaks and Compresses
In uncomplicated superficial folliculitis, if the lesions are very inflamed, your physician might recommend the use of warm compresses to help soothe the area and relieve the itching.
Remember, that these measures must be accompanied by the proper treatment (or lack of) recommended by a specialist.

Treatment #3: Antibiotics and Antifungals
Topical or oral antibiotics can be prescribed by your physician for treatment of folliculitis depending on the condition and severity. In moderate cases that are caused by bacteria, a topical antibiotic can be applied on the affected area daily.
For folliculitis that is more resistant or severe, oral antibiotics can be prescribed for 5 to 30 days. If the doctor determines that your folliculitis is caused by a fungal infection, it can be treated using a topical antifungal or oral antifungal.