What Causes Pancreatic Cancer?
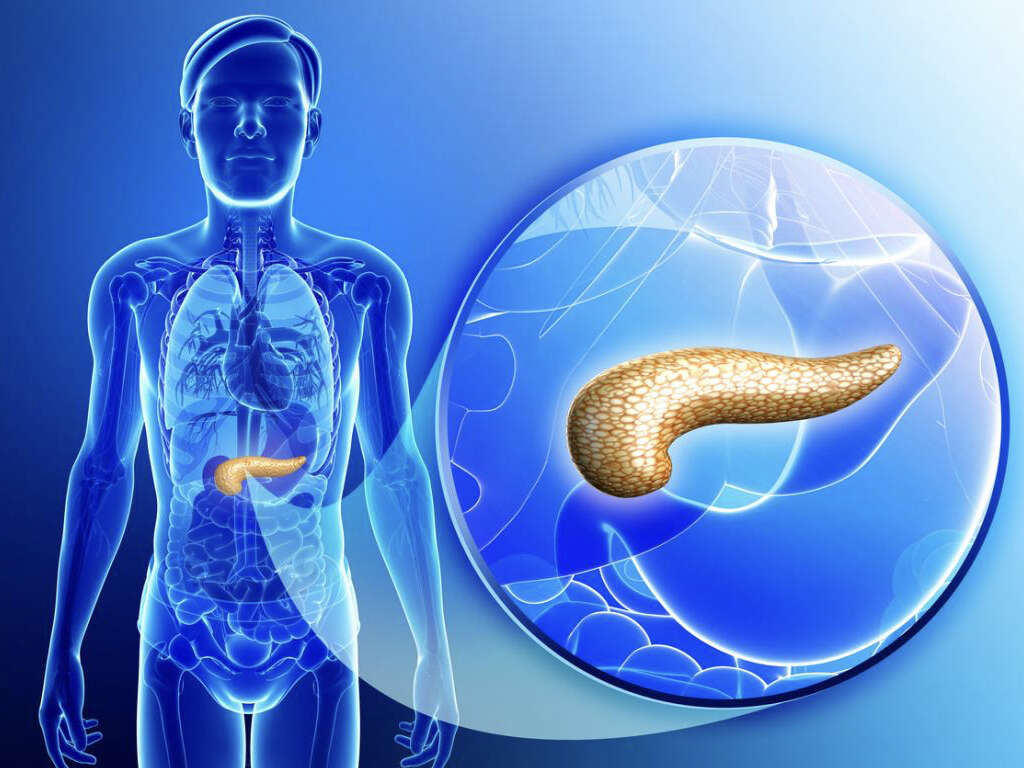
Pancreatic cancer starts when abnormal cells in the pancreas multiply uncontrollably and become a tumor. The pancreas is made up of glandular tissue. It is responsible for production of enzymes that help in the digestion process. It also produces the hormones insulin, glucagon, gastrin, and amylin, which are responsible for controlling blood sugar levels and hunger.
When old cells of the pancreas die, other cells grow to replace them. In some cases, however, new cells form while the old cells still exist. These extra cells multiply to form new tissue where it should not be. Pancreatic cancer is comprised of such tissue. Similar to tumors elsewhere, some pancreatic tumors are benign, which means that they are not cancerous, while others are malignant, which means that they are cancerous.
1. Symptoms of Pancreatic Cancer
Symptoms of pancreatic cancer are usually vague and cannot always be associated with the disease. The symptoms include pain, especially in the abdomen and neck, since the tumor arises in the area between the stomach and the spine, loss of weight, and loss of appetite. Jaundice, with or without itching, may also develop in skin and eyes due to the effects of the disease on the liver. Other symptoms of pancreatic cancer include nausea, changes in stool, inflammation, swelling of the pancreas, and recent-onset diabetes. A person with an advanced case of pancreatic cancer may have depression, general fatigue, weakness, blood clots, and fluids in the abdomen. It is recommended to visit a doctor immediately if you are experiencing some or all of these symptoms.

2. Causes of Pancreatic Cancer
DNA mutations and changes can lead to cancers; whether these changes are hereditary or develop over time. These DNA changes can also happen due to constant exposure to harmful materials such as toxins within the bloodstream. But the cause of pancreatic cancer, similar to other cancers, is not quite clear.
Still, studies indicate that about 10 percent of pancreatic cancers are familial or hereditary. In fact, your risk of getting pancreatic cancer increases if you have two or more close relatives who have, or had, pancreatic cancer.
3. Lifestyle
Smoking, obesity, old age, and other factors may also play a part in the development of pancreatic cancer. When these habits are part of your lifestyle, your chances of getting pancreatic cancer increase further if you have a close relative who has, or had, pancreatic cancer.
A similar scenario applies if you have an inherited genetic syndrome or disease associated with the development of pancreatic cancer.

4. Diseases and Other Conditions Associated with Pancreatic Cancer
There are many chronic diseases and conditions associated with pancreatic cancer. For example, diabetic patients have a higher chance of developing pancreatic cancer than non-diabetics. In fact, diabetes may be a symptom of pancreatic cancer. Long-standing inflammation and swelling of the pancreas or chronic pancreatitis can also be associated with pancreatic cancer.
Tobacco smoking is bad for your body including your pancreas; and any cancer can be associated with this habit. African Americans, Ashkenazi Jews, and people aged 60 years and older have an increased chance of developing pancreatic cancer. Obese people and people who eat a lot of processed foods and meats are also likely to develop pancreatic cancer by the age of 50.

5. Complications of Pancreatic Cancer
Pancreatic cancer does not need any complications to be fatal because it impacts the whole body. This means that if pancreatic cancer is not diagnosed early enough to be treated, it can be fatal. The condition is, however, treatable if discovered early.
Unfortunately, most cases do not survive due to the late diagnosis. The pancreas is located deep in the abdomen and the condition is usually discovered when it is already at an advanced stage.

6. Disease Process
There are two main types of pancreatic tumors and cancers depending on the type of affected tissue: exocrine and endocrine. Exocrine pancreatic tumors and cancers are the most common. They are either benign or malignant but most of them are malignant, meaning they are cancerous.
It can be adenocarcinoma, which starts in the gland cells in the pancreatic ducts, acinar cell carcinoma, which starts in the enzyme cells of the pancreas, ampulla cancer, which starts at the meeting point between the bile duct and pancreatic duct, adenosquamous carcinoma, squamous cell carcinoma, or giant cell carcinoma.
The second type; endocrine pancreatic cancers are less common. They can either be neuroendocrine or islet-cell tumors.

7. Diet and Lifestyle Changes for Pancreatic Cancer Patients
There is no known way to stop pancreatic cancer from developing. However, there are some healthy habits and certain activities that can reduce the risk of developing any kind of cancer including pancreatic cancer. The first thing to do is to stop smoking. Smoking is a major contributing factor to any cancer. Work on your weight so that you have a healthy weight-to-height ratio.
Eat more vegetables, fruits, and whole grains, and eat less red meat and processed foods. Certain vitamins, especially vitamin D, are effective in decreasing the risk of pancreatic cancer. Therefore, make sure that your diet includes vitamin D-rich foods besides other vitamins. Vitamin D helps to regulate pancreatic functions and, hence, improves pancreatic health.

8. Diagnosis
Pancreatic tumors can only be seen through imaging. CT scan, MRI, and endoscopic ultrasound are used to determine the site, size, and extent of the pancreatic cancer. After determining whether the patient has a pancreatic tumor or not, the doctor takes a sample to determine its type, and whether it is benign or malignant. The condition is hard to diagnose since the pancreas is located deep within the abdomen, between the stomach and the spine.
It cannot be felt during a physical examination, and the symptoms are vague. Besides, pancreatic cancer develops over time, and can be misdiagnosed with other health conditions. Diagnosis is, therefore, a complicated process. Still, an early diagnosis can result in treating the condition completely.
9. Treatment
Treatment of pancreatic cancer is complicated. It depends on the type of the tumor, its location, the stage of the condition, the overall health of the patient, and the personal choices of treatment. The first goal is to remove cancer if possible.
If this cannot be done, the goal will be improving the quality of the patients life, and preventing the cancer from spreading to other areas, or growing and causing more problems. Treatment options include surgical intervention, chemotherapy, and radiotherapy. In the late stages, symptomatic treatment and making the patient as comfortable as possible are the main options.
10. Long-Term Outlook
Pancreatic cancer is a life-threating condition that can be difficult to diagnose and treat. The disease is usually discovered late in growth. This is why it is essential to get an early checkup if you have vague or unexplained symptoms in addition to a risk factor or factors of pancreatic cancer.
Early diagnosis and early treatment can give the patient the best possible results. If you are diagnosed with pancreatic cancer, learn more about your condition, and communicate with other people who have conquered their pancreatic cancers. Your family will also come in handy for support as you fight the cancer.