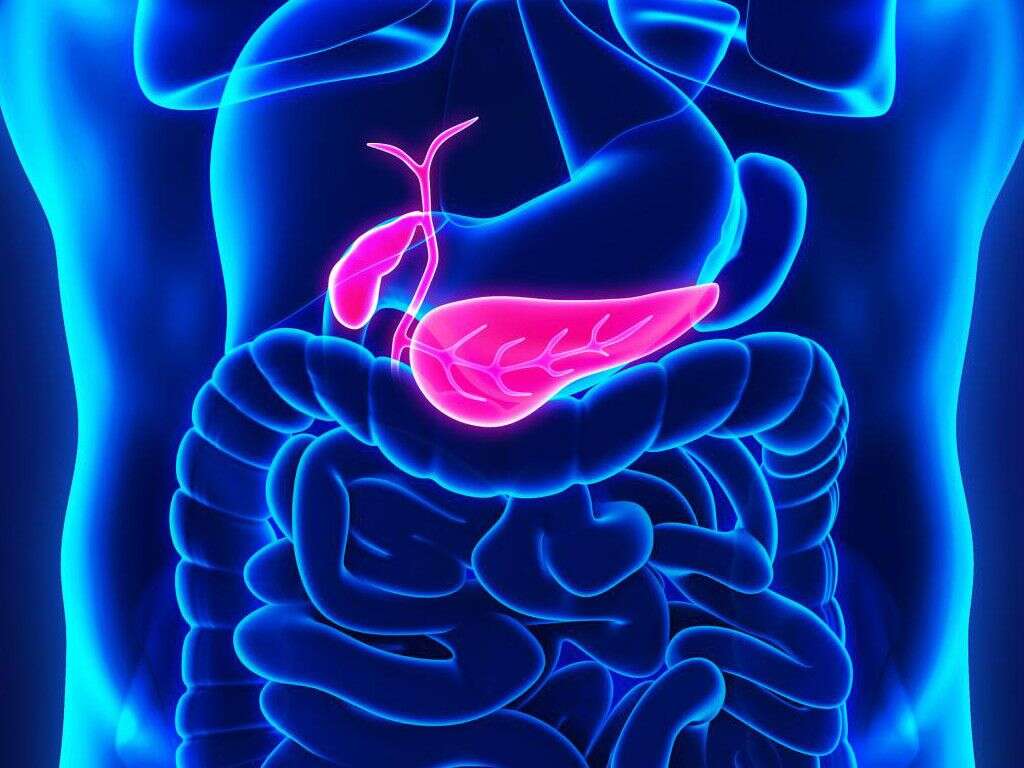
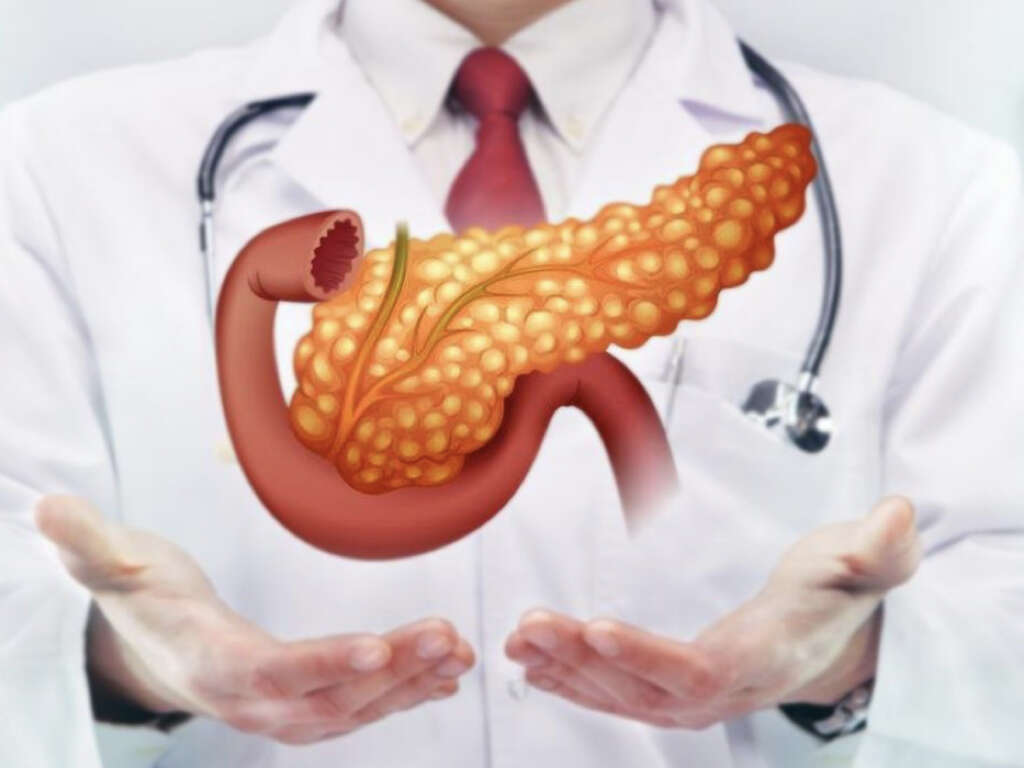
What Does the Pancreas Do?
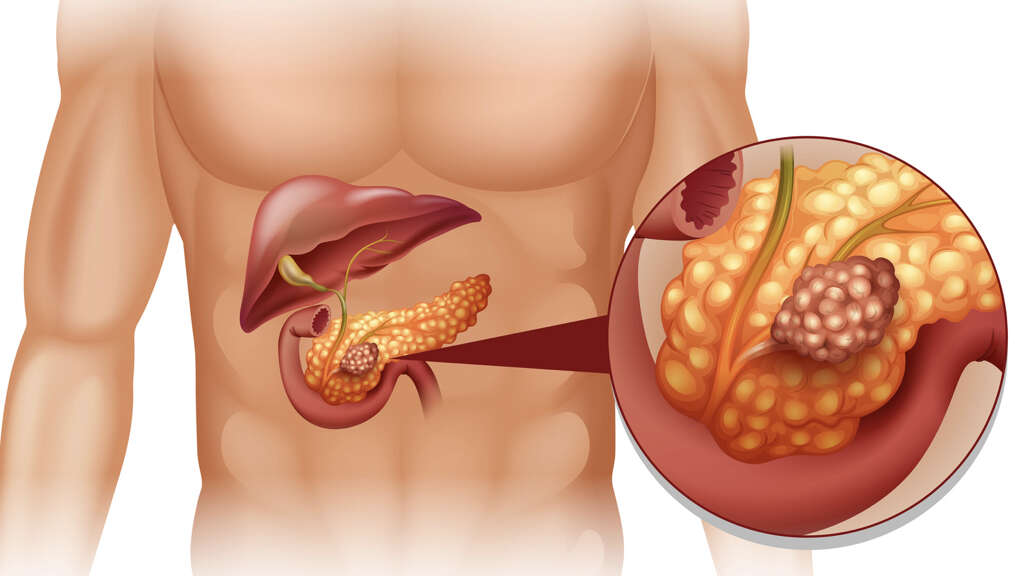
The pancreas is an elongated, flat organ found deep within the middle part of the right side of the abdomen. A portion of it lies between the stomach and the spine, while the rest of it attaches to the curved part of the duodenum. Wider on the right end, the pancreas tapers to a tail-like shape on the other end. The wider part of the pancreas is called the head, the narrowest end is called the tail, and the parts in between are called the neck and the body. The pancreas is about 6 inches long.
The pancreas is an important component of both the endocrine and the digestive functions. It is composed of two main types of functional cells. One type has exocrine functions and produces the digestive enzymes namely protease, lipase, and amylase; the other has endocrine functions and produces the hormones insulin, glucagon, gastrin, and amylin.
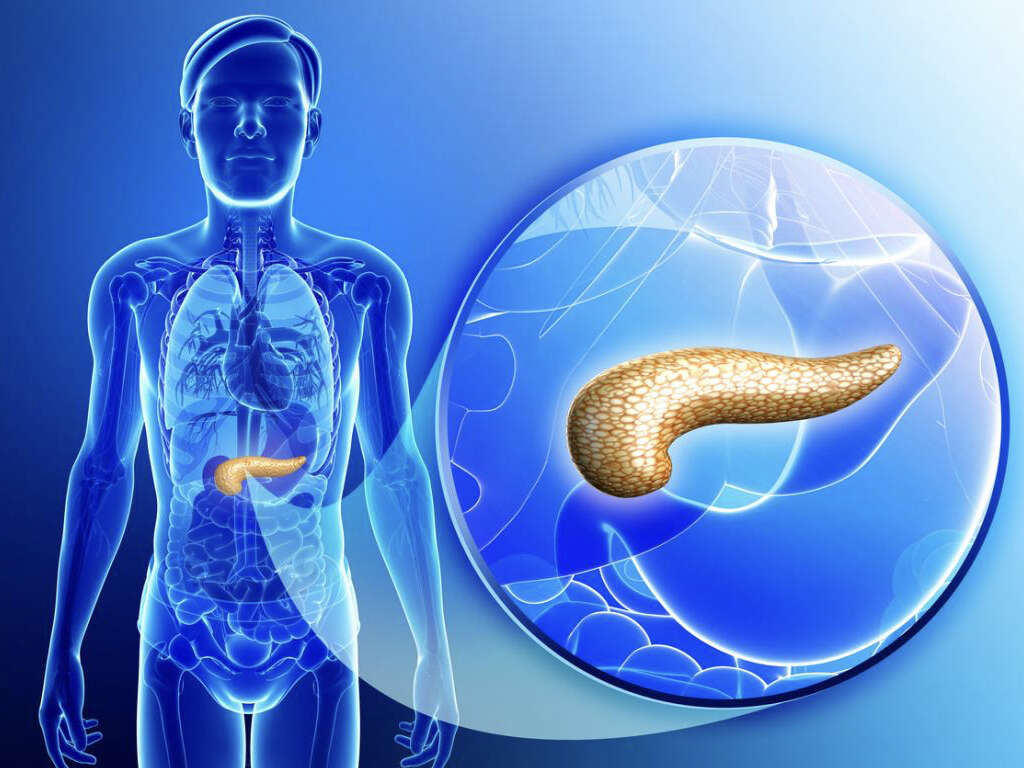
1. Exocrine Pancreas
The exocrine function of the pancreas produces enzymes necessary for the digestion of food. Acinar cells, which carry out exocrine functions, form the bulk of pancreatic tissues. These cells produce the following enzymes: trypsin, chymotrypsin, amylase, and lipase. Once the enzymes are produced, they flow through small ducts that join with others to form progressively larger ducts that lead into the main pancreatic duct.
The pancreatic duct runs through the length of the pancreas, collecting the fluid containing enzymes and transporting it to the duodenum. The three main groups of pancreatic enzymes are protease, lipase, and amylase.
2. Protease Enzymes
Although protein digestion starts in the stomach through an enzyme called pepsin, it is not essential for this purpose. Protein digestion continues in the small intestine with pancreatic enzymes called proteases.
The essential proteases secreted by the pancreas are trypsin, chymotrypsin, elastase, carboxypeptidases A and B. Finally, the digestion is completed by enzymes of the brush border of the small intestine called dipeptidases and aminopeptidases. The end product are amino acids (40%), dipeptides and tripeptides (60%).
3. Amylase Enzyme
Carbohydrate is the main source of energy in humans and many animals, but starch cannot be absorbed into the body in its raw form. Amylase is the enzyme that breaks down starch into a simpler form for absorption.
Alpha-amylase is a pancreatic enzyme that breaks down starch into oligosaccharides and disaccharides (i.e. lactose, maltose). These molecules are later broken down by brush border enzymes (maltase, lactase, sucrose-isomaltase) of the intestine into monosaccharides (glucose). In the late duodenum and early jejunum, monosaccharides are finally absorbed by diverse mechanisms.
4. Lipase Enzyme
In general, fat molecules cannot be absorbed into the bloodstream in their raw forms. Triglyceride digestion starts in the stomach where fatty materials are pulverized to small particle sizes to increase surface area for faster digestion.
In the small intestine bile micelles emulsify the fat by causing it to break down into smaller units (emulsification), to increase the surface area on which the lipase can actually act on. The pancreatic lipase acts on these emulsion droplets, converting them into two major end products: 2-monoglycerides and fatty acids.
5. Bicarbonate
Bicarbonate may not be an enzyme but, being a base, it necessary for neutralizing gastric acid. Once gastric acid has carried out its digestive roles, it must be neutralized so that it does not cause injury to the intestinal walls. Unlike the stomach walls, intestinal walls are not protected against this injury.
Therefore, an enzyme named secretin is released from the duodenum in response to acid entering the stomach. Its action on the pancreas is the release of fluid high in bicarbonate.

6. Endocrine Pancreas
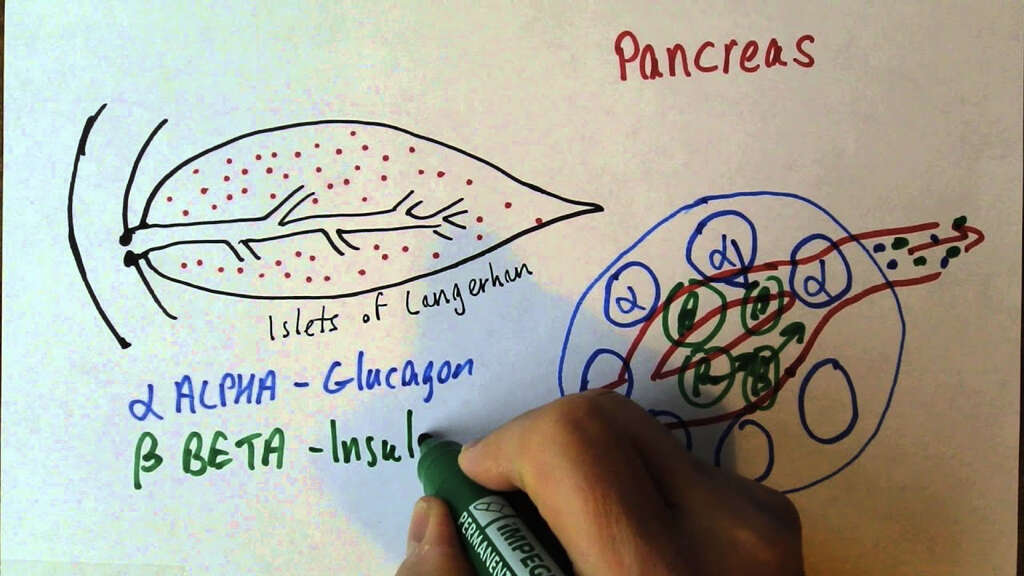
The endocrine part of the pancreas is called the pancreatic islets or the islets of Langerhans. These are clusters of cells spread throughout the pancreas. The islets are comprised of four types of cells in which the four pancreatic hormones are produced.
The four types of cells are alpha cells, beta cells, delta cells, and PP cells. Alpha cells secrete a hormone known as glucagon. They tend to be located near the periphery of the islet and constitute about 20 percent of the islet cells. Beta cells synthesize preproinsulin, a precursor of a hormone called insulin. They constitute approximately 60-75 percent of the islet cells. Finally, delta cells constitute 5 percent of the islet cells, and secrete somatostatin.
7. Insulin Hormone
Insulin is a hormone that controls blood glucose levels by aiding the entry of glucose molecules into the cells of different tissues. Insulin production usually increases after a meal, when the level of glucose in the bloodstream rises. Conversely, the production decreases when blood glucose levels dip. However, if the pancreas is not functioning properly, production of insulin may be affected. This can interfere with the absorption of glucose by cells such that blood sugar levels rise (hyperglycemia). In many cases, this leads to diabetes mellitus.
The tissues that require insulin for glucose uptake are adipose tissue (fat), skeletal muscle, and liver. In these tissues insulin has anabolic effects (building-up instead of breaking-down aspect of metabolism). For example, in the liver, insulin promotes glycogen synthesis or glycogenesis (the main form of storage of glucose in the body), increases protein synthesis, and triglyceride synthesis (lipogenesis). At the same time, it inhibits the breakdown of glycogen (glycogenolysis), fats (lipolysis)and proteins in these tissues.
8. Glucagon Hormone
Glucagon is a hormone synthesized by pancreatic alpha cells, in response to hypoglycemia or a low concentration of glucose in the blood (i.e. fasting). Conversely, high plasma glucose (hyperglycemia) is its most important inhibitor.
The primary target for glucagon action is the liver, where it increases glycogenolysis (break-down of glycogen into glucose) and gluconeogenesis (de novo synthesis of glucose) in order to release glucose into the bloodstream. It also increases the production of ketone bodies and decreases lipogenesis (triglyceride synthesis) in the liver. As you can probably notice by now, this means that glucagon does the exact opposite of what insulin does. Glucagon and insulin work “together” to control blood sugar levels.

9. Somatostatin Hormone
Pancreatic somatostatin hormone is produced by the delta cells in the islets of Langerhans.
This hormone inhibits the production of both insulin and glucagon. It can also decrease acid production in the stomach directly or indirectly. Other forms of somatostatin hormone are produced in other sites in the body including the brain (hypothalamus).

10. Pancreatic Peptide Hormone
Pancreatic polypeptide hormone is produced in the PP cells in the islets of Langerhans in the pancreas, which comprise about 1 percent of the cells in the pancreatic islets.
The role of the pancreatic peptide hormone includes control of appetite, as well as the regulation of the endocrine and exocrine functions of the pancreas.