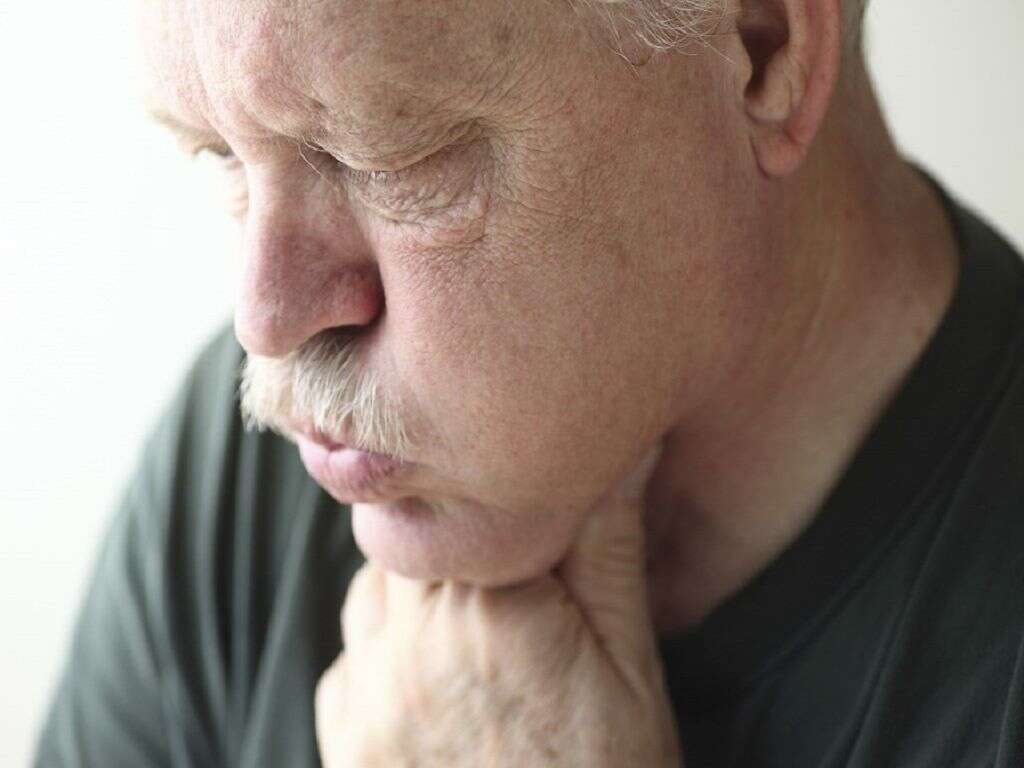
What Is Hashimoto's?
There are four main types of thyroid disease: hyperthyroidism, hypothyroidism, benign thyroid disease, and thyroid cancers. Hashimoto’s disease, also known as Hashimoto thyroiditis, is a type of hypothyroidism in which the functioning of the thyroid gland is diminished. It is named for a Japanese surgeon who first described the condition in 1912.
If you are experiencing fatigue and weight gain, you may be curious whether hypothyroidism could be to blame. If you have been diagnosed with Hashimoto’s, you may have questions about treatment options and what to expect. Here are 10 important facts to know, based on frequently asked questions about this condition.

1. Cause
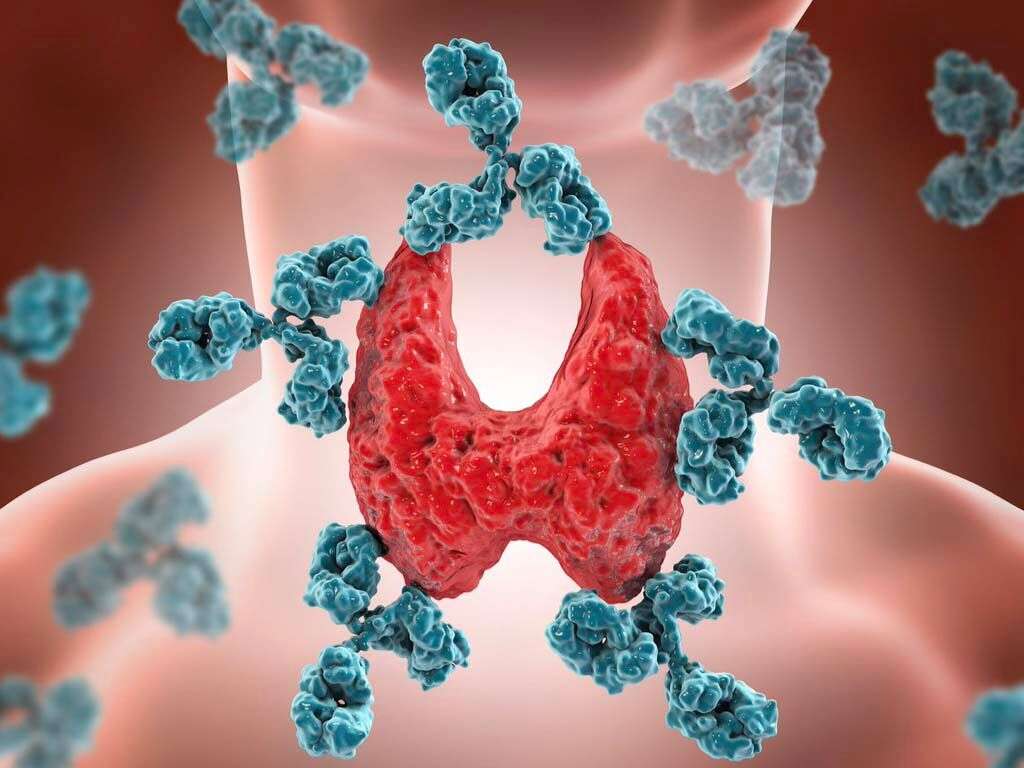
Hashimoto’s disease is one of several autoimmune thyroid diseases in which the body’s immune system destroys cells of the thyroid gland or blocks its production or secretion of hormones. Specific antibodies that attack thyroid cells include anti-thyroid peroxidase, antithyroglobulin, thyroid-stimulating antibody, cytotoxic antibody, and TSH receptor-blocking antibodies.
The disease has a genetic component, so a person is more likely to develop it if other family members have previously been diagnosed. Environmental triggers that increase risk are cigarette smoking, excess dietary iodine, chemicals such as BPA, medications such as lithium or amiodarone, antiretroviral therapy, and chronic or acute stress.
2. Early Warning Signs
Before being diagnosed, or sometimes before even suspecting thyroid trouble, many people experience early warning signs of the disease. At their onset, these symptoms are subtle and easily attributable to other causes. As they increase in severity over months or years, they eventually lead people to seek information and help.
In retrospect, many patients with Hashimoto’s disease realize they had not felt well for some time. Most report feeling chronically tired, and blame the weight they have gained on a lack of energy. Other early symptoms include constipation, dry skin, and brittle hair. Some notice an increased sensitivity to cold.

3. Symptoms
As the disease progresses, symptoms become more pronounced. Lack of thyroid hormone affects other organs in the endocrine system that rely on negative feedback loops for proper functioning. Potential problems include galactorrhea, infertility, and irregular menstrual cycles in women. Cardiovascular symptoms include high blood pressure and bradycardia.
Chronic fatigue worsens over time, leaving some people feeling depressed. Effects on the brain can cause dementia, memory loss, or other psychiatric conditions. Sleep apnea is common. Other problems of the nervous system lead to neuropathy, joint pain, and nerve deafness.
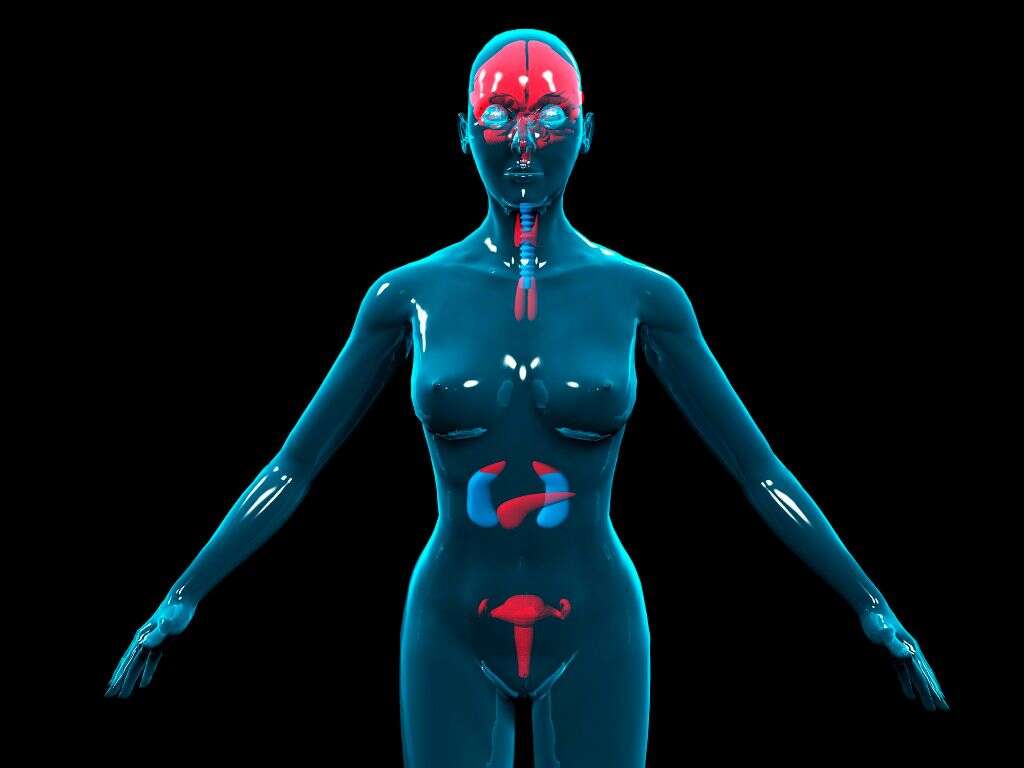
4. Physical Appearance
People with advanced Hashimoto’s disease gain weight, and their faces appear puffy, especially around the eyes. Their hands and feet are often swollen. The skin is dry, and their nails are thick, brittle, and ridged. They have thin, wispy hair and eyebrows.
Because of its effects on the nervous system and joints, people with Hashimoto’s disease move slowly or with difficulty. An enlarged thyroid, or goiter, may be visible in their necks and might also cause them to speak slowly, or with a hoarse voice. Sometimes they may appear confused or forgetful.

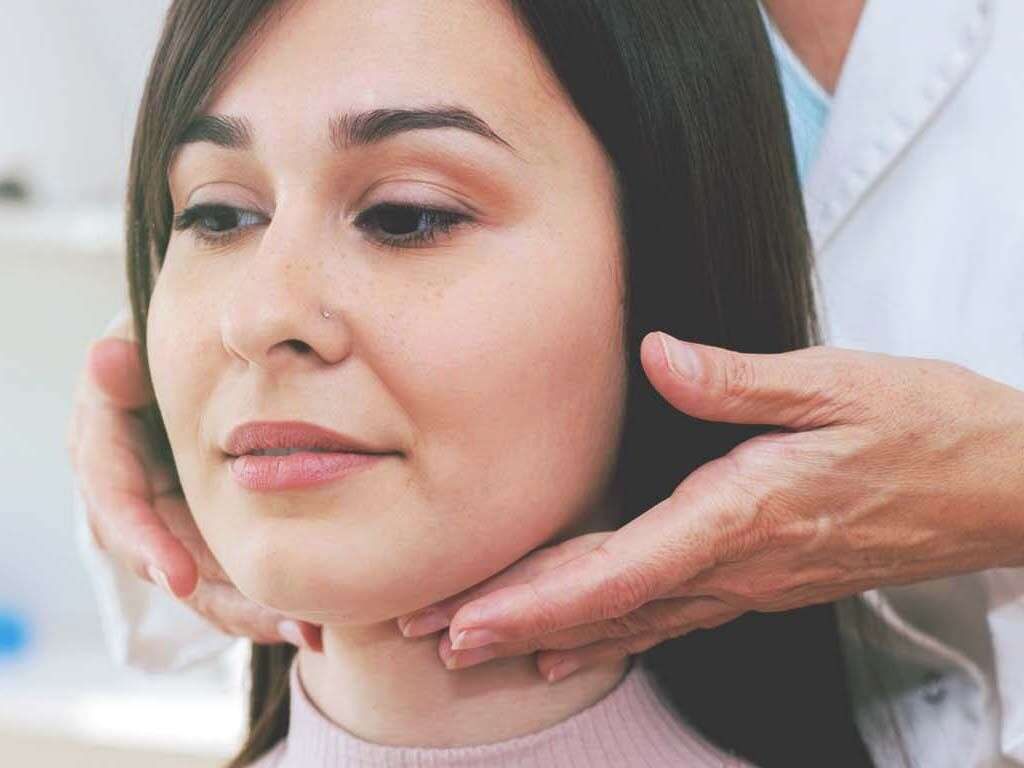
5. Diagnosis
Doctors who suspect thyroid trouble will recommend a blood test to measure the level of serum thyroid-stimulating hormone. This hormone is elevated in those with hypothyroidism. They also will test for levels of T3 and T4, and the presence of thyroid autoantibodies.
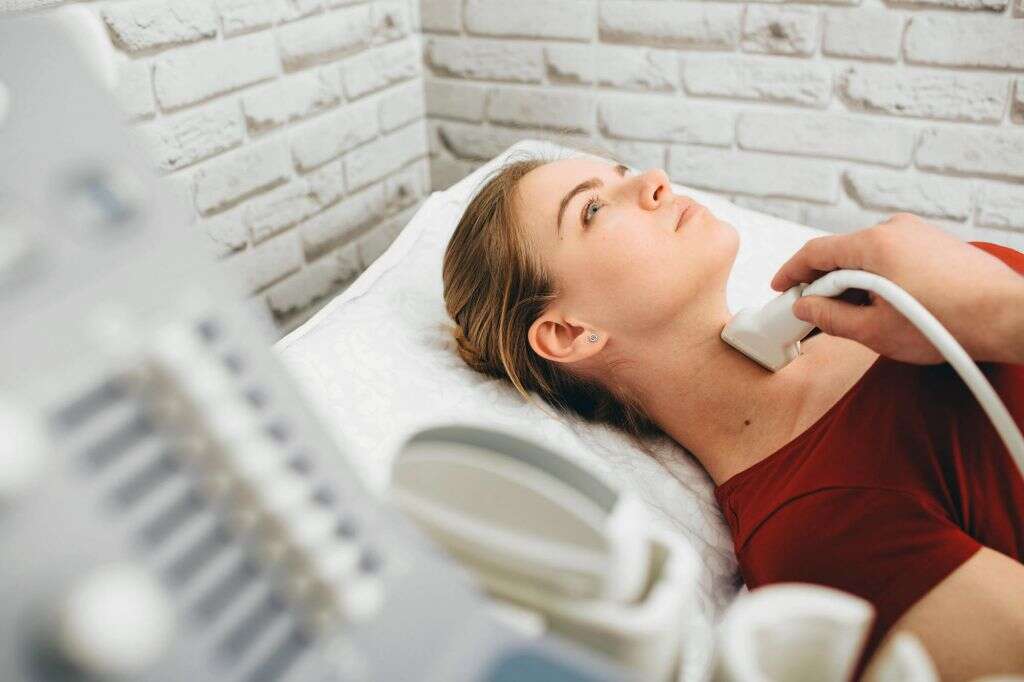
Ultrasound imaging allows a doctor to measure the thyroid and to detect any nodules that might be present. If the thyroid has enlarged dramatically or if there are nodules inside, a doctor may perform a biopsy to test for cancerous cells.
6. Treatment
The prescription medication usually given to treat Hashimoto’s disease is levothyroxine sodium. Pharmacists must titrate this drug for each individual, based on frequent checks of thyroid hormone levels in the blood. The patient must take this oral medication daily for the rest of his or her life.
Natural health practitioners recommend changes to diet and lifestyle to support thyroid health. The main focuses of this approach are healing any bowel or digestion issues and reducing stress. For some, these alterations alone are enough to manage Hashimoto’s; other people must combine them with thyroid medication.

7. Surgery
In some cases, doctors remove part or all of the thyroid. They typically only recommend this surgery in extreme cases, such as when a goiter is so large that it prevents the patient from eating, speaking, or talking normally. The presence of malignant nodules or lymphomas also warrants surgical removal.
Some patients prefer to have a thyroidectomy for cosmetic reasons. Some surgeons will consent to remove large, unsightly goiters, while others will do the procedure only when it is medically necessary. A patient who has had the thyroid removed must take medication to compensate for not being able to produce his or her own thyroid hormones.
8. Occurrence
Of autoimmune diseases that affect specific organs, autoimmune thyroid disorders are the most common. They affect 5-15% of women and 1-5% of men in the United States. Some people are born with hypothyroidism, while some develop it later in life. Iodine deficiency is thought to contribute to hypothyroidism’s prevalence in some parts of the world.
In the U.S. and other countries with sufficient dietary iodine intake, most cases of hypothyroidism after age 6 are due to Hashimoto’s disease. Worldwide, experts believe it to occur in 0.3-1.5 people in every thousand. Many additional cases, however, probably go undiagnosed.
9. Prevention
Because Hashimoto’s disease can be inherited, it is important to know your family’s medical history. One study found that having a close relative with the condition makes people nine times more likely to develop it themselves. However, having a genetic predisposition to an illness does not guarantee that it will manifest. There are many lifestyle choices people can make to minimize their risks.
Avoiding cigarette smoke and other sources of cyanide is extremely important. Other substances that adversely affect the thyroid are excess dietary iodine, radioactive materials, bisphenol-A, antiovulatory birth control medications, and chemicals released from non-stick cookware. Deficiencies of vitamin D3 and selenium are associated with increased risk, so some nutritionists recommend supplementing with these nutrients.

10. Related Conditions
People with Hashimoto’s thyroiditis are more likely also to have certain other autoimmune disorders. These conditions include type 1 diabetes, pernicious anemia, adrenal insufficiency, and celiac disease, as well as various types of arthritis and connective tissue diseases. Children and adolescents are more likely to have diabetes and celiac disease, with the other conditions being more prevalent in adults.
The above-mentioned conditions may be present before the diagnosis of Hashimoto’s or patients may develop them later. Because 30-40% also are anemic, some doctors routinely perform a complete blood count. Other tests to diagnose potential comorbidities include a lipid profile, basic metabolic panel, creatine kinase levels, and prolactin levels.