Pink Eye Causes, Symptoms & Treatments
Pink eye or conjunctivitis is the inflammation of the conjunctiva, a layer of tissue that covers the eyeball and reflects back forming the inner layer of the eyelid. It is one of the commonest non-traumatic eye presentations in the emergency department. It constitutes about 1% of primary care practitioner office visits in the United States and affects approximately 6 million people every year.
Conjunctivitis can occur when the infectious agent adheres to the conjunctiva. Classification of conjunctivitis is based on the offending pathogen, age of occurrence, or progression of disease. Most cases of conjunctivitis will resolve spontaneously. However, depending on the immune status of the affected individual and offending pathogen, it can sometimes lead to severe infections that threaten vision. Conjunctivitis can affect all individuals regardless of age or gender. Let’s explore some of the common causes, symptoms and treatments of pink eye:

Cause #1: Viral Conjunctivitis
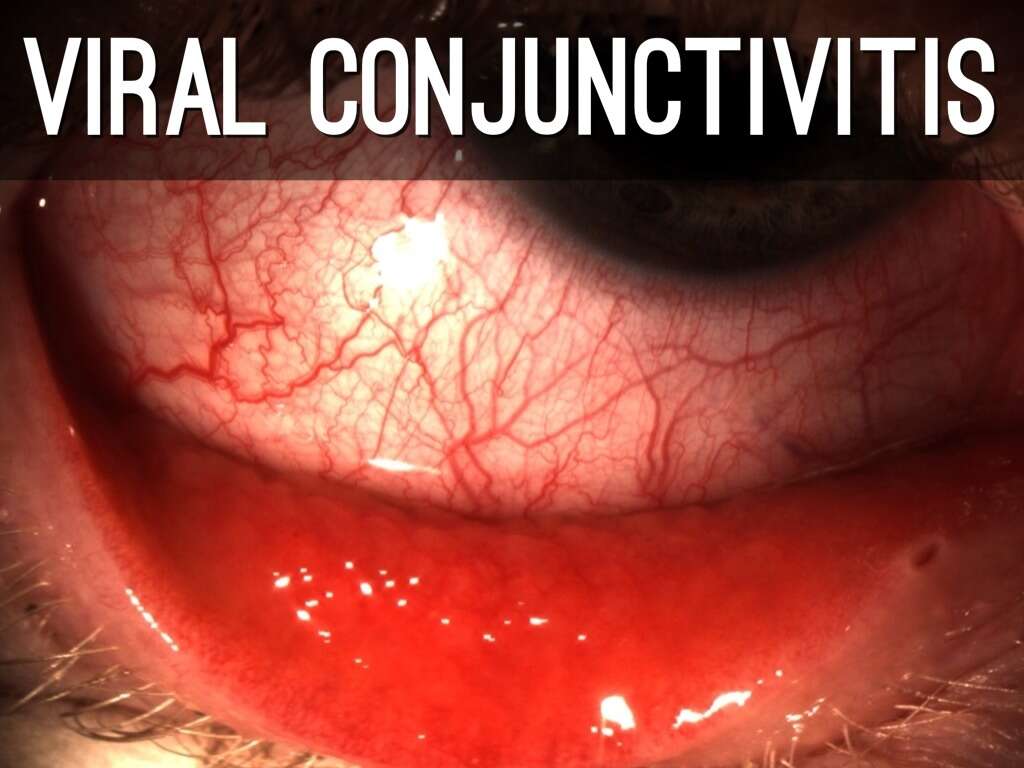
Viral conjunctivitis is usually caused by the adenovirus. Other viruses that can cause pink eye are the varicella zoster virus, herpes simplex virus, picornavirus (such as certain strains of coxsackie and enterovirus), poxvirus (such as vaccinia virus and molluscum contagiosum), and human immunodeficiency virus (HIV).
Conjunctivitis that is caused by a viral infection is very contagious. Contagion starts from the onset for as long as 10 to 12 days as long as the eyes remain pink or red. To prevent spread and transmission, patients should avoid touching their eyes and contact with others. The infection will usually resolve on its own within two to four weeks.
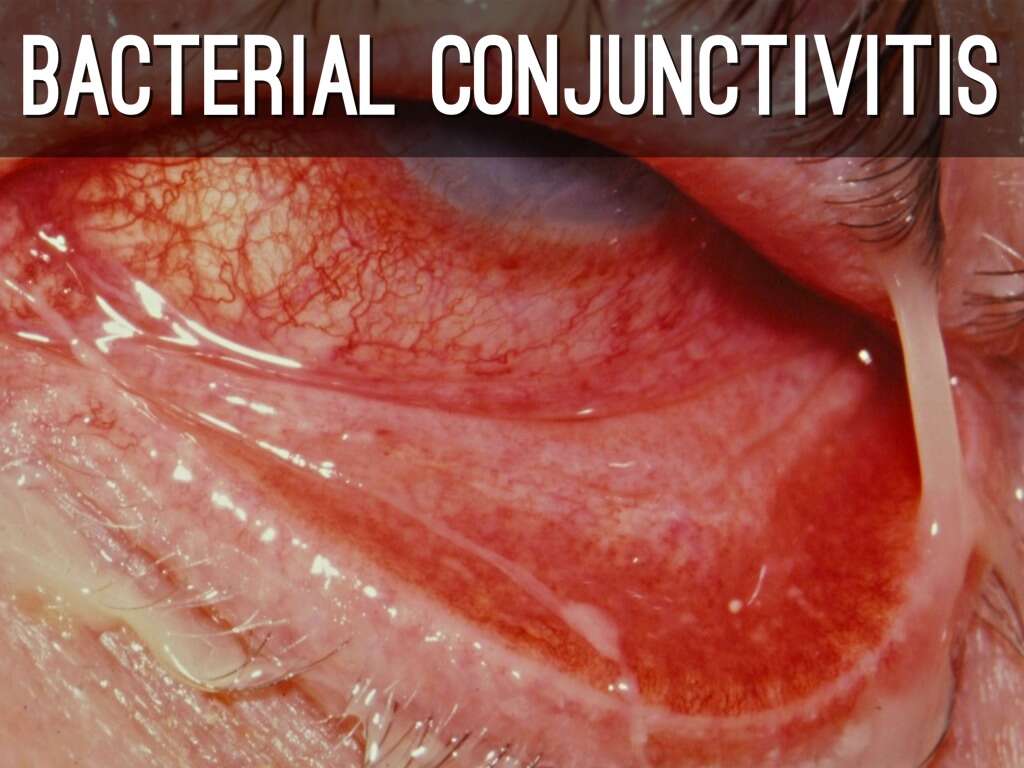
Cause #2: Bacterial Conjunctivitis
About 30% of patients with acute conjunctivitis seeking primary care, turn out to be bacterial in origin. In the United States, it is estimated to cost between $377-875 million in healthcare costs. The commonest bacteria that can cause bacterial conjunctivitis are Staphylococcus, Streptococcus, Haemophilus, Pseudomonas, Corynebacterium, and Moraxella species.
Complications from bacterial conjunctivitis can be more severe, ranging from mild irritation to severe cases including vision loss. Severe cases are usually caused by very harmful bacteria such as Neisseria gonorrhea and chlamydia trachomatis.
Cause #3: Allergic Conjunctivitis
As the name suggests, allergic conjunctivitis is caused by allergies. There is usually no pain or history of exposure to offending pathogens. Allergic conjunctivitis can be categorized into 5 categories: seasonal allergic conjunctivitis (SAC), perennial allergic conjunctivitis (PAC), vernal keratoconjunctivitis (VKC), giant papillary conjunctivitis (GPC) and atopic keratoconjunctivitis (AKC).
VKC is a more aggressive form in children while AKC occurs in adults. VKC in children mostly affects young boys, involves both eyes, and usually happens when there is warm weather. Allergic conjunctivitis usually resolves on its own and rarely has complications. Early treatment can help prevent it from worsening.
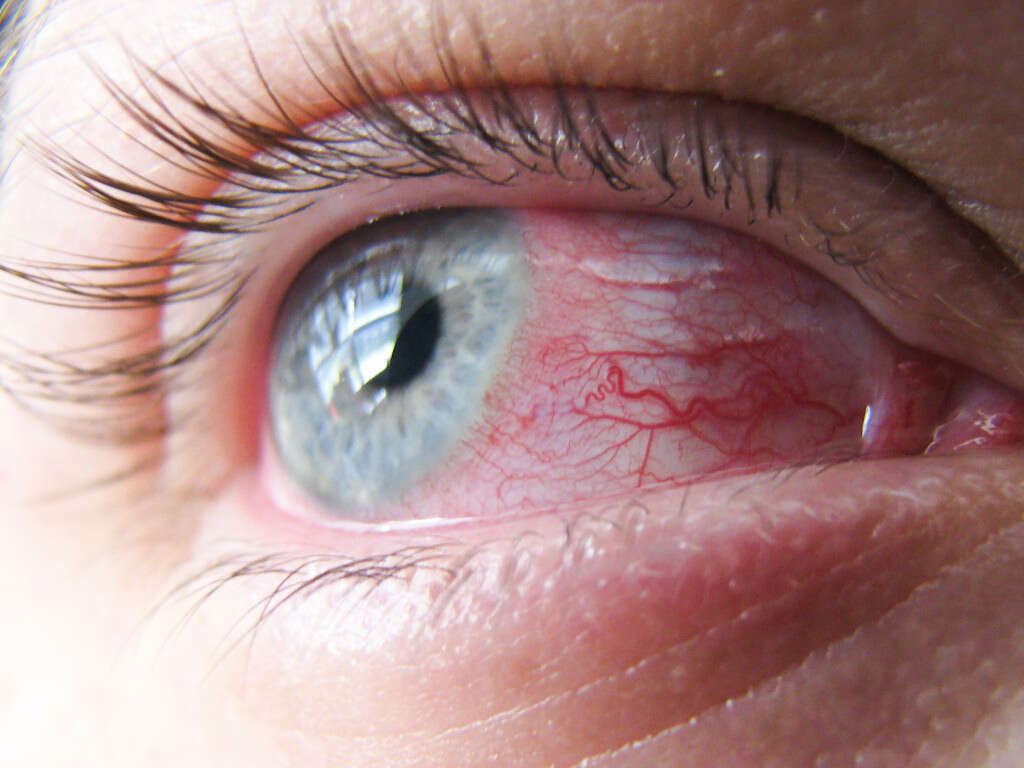
Symptom #1: Redness
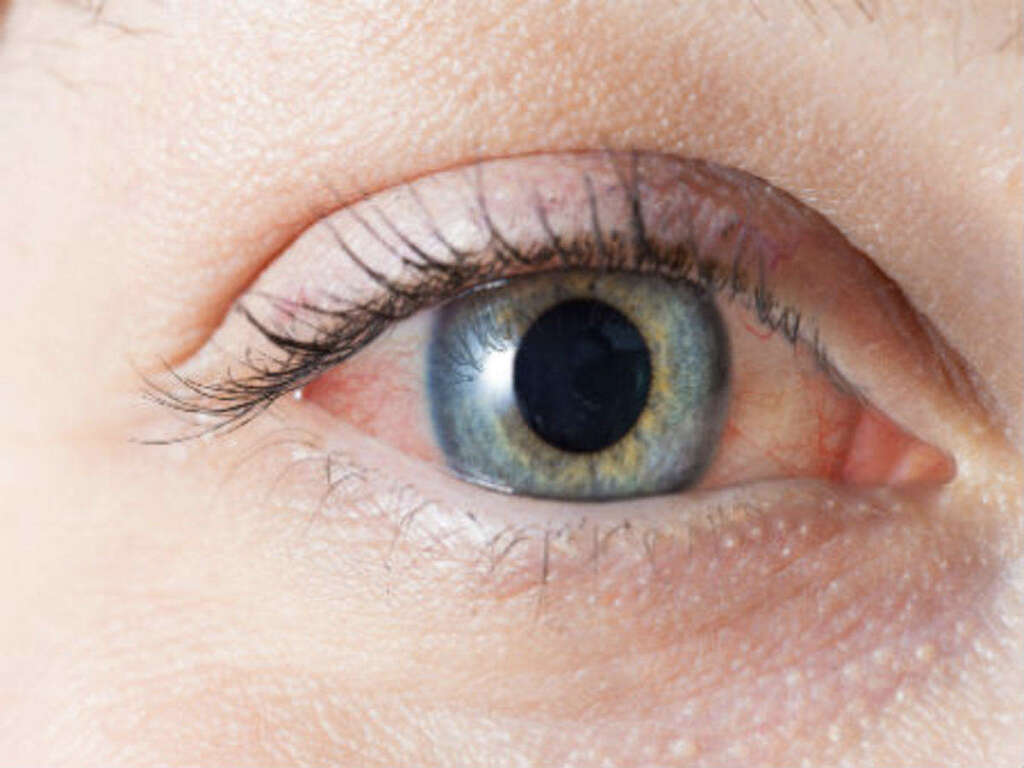
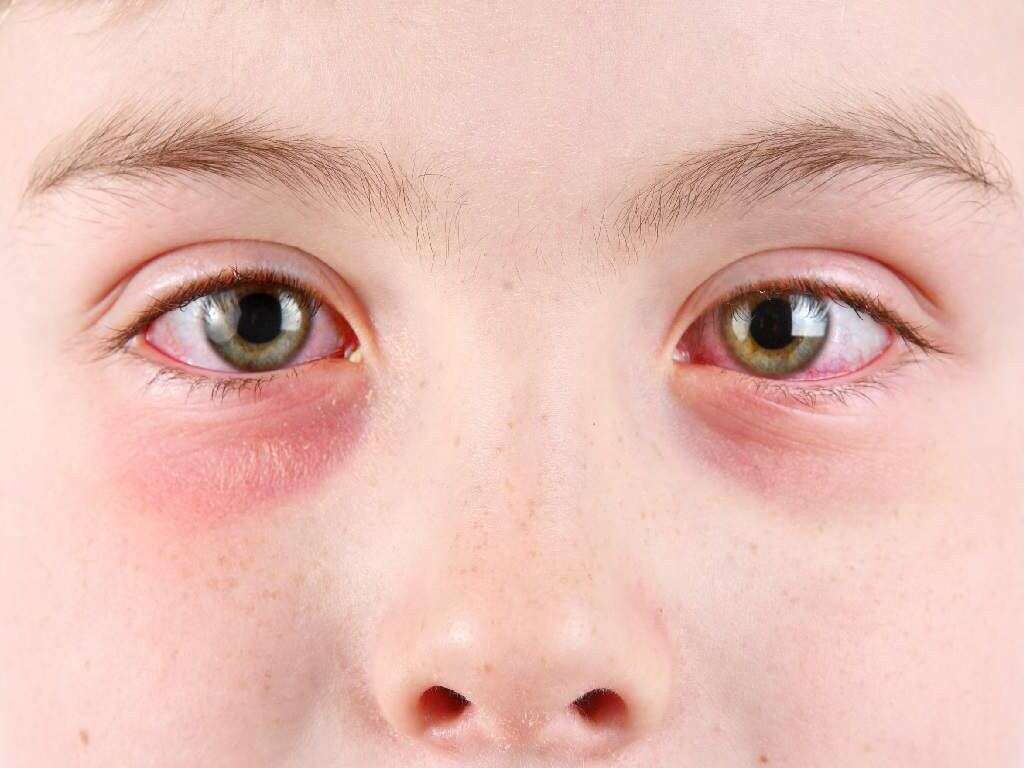
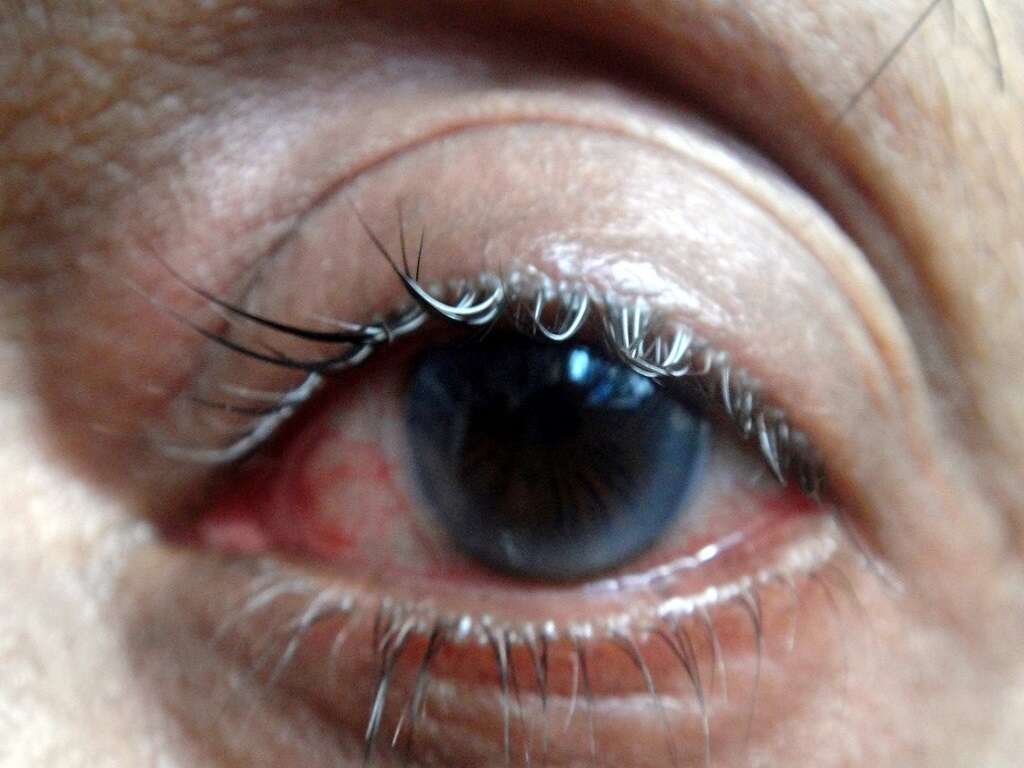
One of the classic characteristics of pink eye is the reddish or pinkish tint of the eye. The previously white area in the eye is now red or pink, looking as if the affected individual has been crying. This occurs due to the inflammation and irritation of the conjunctiva. It can affect one or both eyes.
In most cases, it often starts in one eye and spreads to the adjacent eye. The redness and irritation will resolve once the infection has cleared. Patients are advised not to touch their eyes as it increases spread and transmission to the other eye and other people.

Symptom #2: Discomfort
When you have pink eye, there can be discomfort in the affected eye. Some patients describe it as a hot and burning sensation, pain, itchiness, or a sensation that there is a foreign item in the eye. The affected eye can also be more sensitive during this time to smoke, fumes and household chemicals.
Depending on the cause of your conjunctivitis, there can be tearing and swelling as well. If your doctor has determined your conjunctivitis to be caused by allergies, avoid exposure to the allergen.
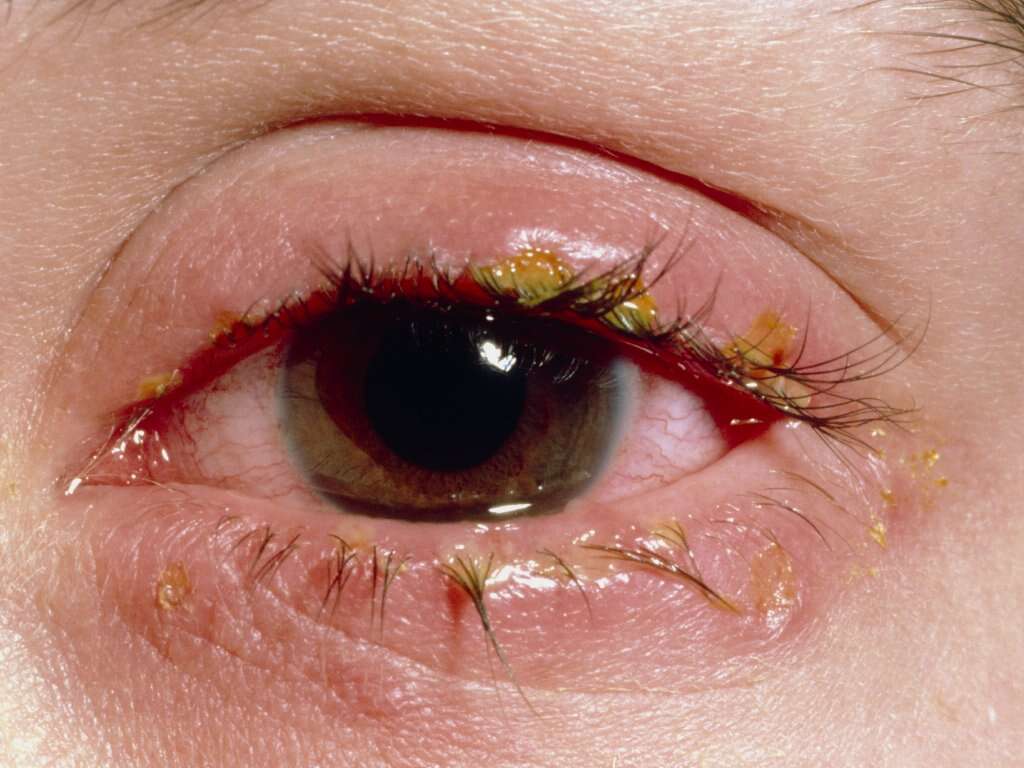
Symptom #3: Discharge
In some cases of conjunctivitis due to bacterial infection, there can be a discharge from the eye. In bacterial conjunctivitis, the discharge is mucopurulent and usually starts in one eye. It may spread to the other eye two to five days later. If the conjunctivitis is caused by pyogenic (produces pus) bacteria, the affected eye can feel gritty and irritated.
The discharge can be described as stringy, greyish, or yellowish that causes the eyelids to stick together especially when waking up in the morning. The infected eye is often crusted. Some patients may insist that there is a foreign item in the eye and cases can be very painful.
Treatment #1: Antihistamines
Antihistamines are a class of drugs that can be used in the treatment of allergies. Topical or oral antihistamines can be used to help relieve symptoms such as itchiness. Oral antihistamines may cause minor side effects such as dry mouth and drowsiness.
Topical antihistamines can help relieve redness and itching of the eyes. Some of the antihistamines used include epinastine and azelastine which start working relatively quickly and are effective in allergic conjunctivitis.

Treatment #2: Topical Antibiotics
Topical antibiotics that have a broad spectrum can be used in mild cases of conjunctivitis. In mild and non-threatening cases, older antibiotics such as trimethoprim with polymyxin B, azithromycin, gentamicin, tobramycin, neomycin, ciprofloxacin can be used.
Newer antibiotics such as the latest fluoroquinolones (moxifloxacin, besifloxacin, levofloxacin) should be avoided and only used in serious cases to reduce bacterial resistance. Rarely will serious cases require the patient to be admitted to receive consistent antibiotics (fortified aminoglycoside cephalosporin combination therapy, topical fluoroquinolone monotherapy) every fifteen to sixty minutes.
Treatment #3: Virus Specific Treatments
Virus specific treatments depend on the type of virus causing the conjunctivitis. In an adenoviral infection, povidone-iodine 0.8% can be used to reduce contagion. In a herpes simplex virus infection, topical antiviral gels such as the ganciclovir gel or vidarabine ointment may be used. A varicella zoster virus infection requires the use of oral acyclovir, valacyclovir, or famciclovir to stop the virus from replicating. A molluscum contagiosum infection will require the treatment of the primary skin lesion where the central core has to be removed.
Other viral causes are usually self-limiting and resolve spontaneously. Supportive treatment with warm compresses, cool compresses, or chilled artificial tears can be used to provide comfort and relief of symptoms.
In all cases you should not self-treat, but instead seek the expert medical advice of a physician.